TUCSON, Ariz. – Even though Agnes Attakai is a longtime Indian health administrator, she had no way of knowing that her Diné family members would become a textbook illustration of Native America’s disadvantages in facing the Covid-19 pandemic.
Then she was forced to say goodbye to two aunts, an uncle and a cousin who succumbed to Covid-19 within three weeks of each other following the Thanksgiving Day holiday. She experienced first-hand the losses that are an all too common story among many Native American families.

Releasing the most recent in a plethora of reports on Covid-19 rates by race and ethnic markers, the Centers for Disease Control showed American Indian and Alaska Native people are 3.7 times more likely to be hospitalized from Covid-19 than Asian and non-Hispanic persons, as well as 2.4 times more likely to die from it.
These are the highest rates of any racial or ethnic group represented in the study. Data from the CDC and other health agencies have shown this kind of wide disparity since the beginning of the pandemic.
As is true with so many families, Attakai’s was not able to hold the hands of their loved ones battling the coronavirus.
“We were on Zoom with him for almost eight hours,” she said, describing her uncle’s final moments. “We talked to him and played his favorite songs,” she told the Native Sun News Today.
She described his grandchildren looking on from behind a glass barrier, knocking on it to let him know they were there.
Attakai is the director of Health Disparities Outreach & Prevention Education at the University of Arizona.
She said the outsized hospitalization and death rates among AI/AN people can largely be attributed to underfunding of the Indian Health Service (IHS) and resource allocation.
“Depending on where you go, you might have really good care, other places you might not,” she said. She added that funds are distributed to IHS facilities differently and that many do not provide emergency or inpatient services.
“We’ve heard, per-capita early on in this pandemic, that the Navajo Nation was No. 1 in the country for Covid-positive cases…. Now we are No. 1 per capita in the country for administering vaccines.”
— Navajo President Jonathan Nez
“Many times, they can’t treat Covid-19 patients in the facilities,” she said. “If patients had milder symptoms, they would treat them but everyone else was transported out.”
She said Navajo tribal members with severe Covid-19 symptoms are often transported to non-IHS facilities in Tucson, Phoenix and Albuquerque, at which they may not have full coverage.
In response, some IHS clinics in the Navajo Nation started utilizing available building spaces and pop-up tents for urgent care so they could separate Covid-19 patients from everyone else.

January 2021
Attakai added that the tribe has paid for motel stays for those who are Covid-positive, in order to help keep people – often living in multi-generational homes — quarantined.
Jo Carrillo, law professor and Director of the Indigenous Law Center at UC Hastings, agrees that the underfunding of the IHS is a major factor in these disparities. She cited a 2017 New York Times report that found that IHS funding allows for roughly $3,000 per patient per year compared with $13,000 for the general population on Medicare, and $7,700 for those on Medicaid.
“These [IHS] allocations were insufficient in 2017 and they’re certainly insufficient for the Covid emergency today,” she said. “The IHS, in my view, is part of the story of Covid’s impact on Native American and indigenous communities.”
According to an analysis by the National Congress of American Indians, IHS funds would have to double in order to match the average healthcare allocation for federal prisoners.
“The IHS has been underfunded from the start,” said Jonathan Nez, President of the Navajo Nation. “Because of that underfunding, there is limited resources going out to the Navajo Nation and all 574 tribes throughout the country.”

January 2021
He said that 29,000 Navajo people have tested positive for the novel coronavirus, and over 1,000 people have died from it.
In addition to IHS funding issues, other infrastructure factors affect Covid-19 rates among many Native Americans.
Some 30-40 percent of Navajo citizens have no running water. ‘They don’t have electricity as well,” said Nez. “When we were hoping for relief to come from the federal government, the first citizens of this country had to wait and actually file a lawsuit for our share of resources.”
He referred to the federal government’s delay early in 2020 in distributing $8 billion of CARES Act funds set aside for tribal members. In May, six tribes filed a lawsuit to force the U.S. Treasury to distribute the funds.
Tribe-owned business’ closures also have impacted Native communities’ ability to fight the effects of Covid-19.
“Most tribal communities do not have a tax base and they depend upon businesses run by tribal entities,” said Attakai. “Due to Covid and the stay-at-home orders, a lot of businesses were shuttered.” She said the temporary closure of casinos in particular has hit hard.
“The gaming industry employs a lot of Native folks in the community. Most of my relatives work in some of those facilities,” she said. “Funds that come from gaming go into tribal coffers to help fund law enforcement, education, health care and other critical services.”
Despite the many systemic challenges that tribes face in keeping their communities safe during a pandemic, one bright spot has been the rollout of Covid-19 vaccinations.

January 2021
The Urban Indian Health Institute recently released a report stating that 75 percent of American Indians and Alaska Natives are willing to get vaccinated, compared to roughly 60 percent in the rest of the population.
The study found that the main reason given for willingness to vaccinate is a sense of responsibility to the community and future generations.
“We’ve put 74,845 shots into the arms of our Navajo citizens,” said Navajo President Nez. “We’ve heard, per-capita early on in this pandemic, that the Navajo Nation was No. 1 in the country for Covid-positive cases…. Now we are No. 1 per capita in the country for administering vaccines.”
Attakai said that the Navajo Nation’s choice to receive vaccinations directly from the federal government as opposed to the state has helped make the rollout more efficient. She added that massive education efforts have also played a major role.
“They’ve really been putting out the information regarding the value and importance of vaccinations,” she said. “And of course, families have been hard-hit.” She said the many losses in Native American communities have made people hungry for the vaccine.
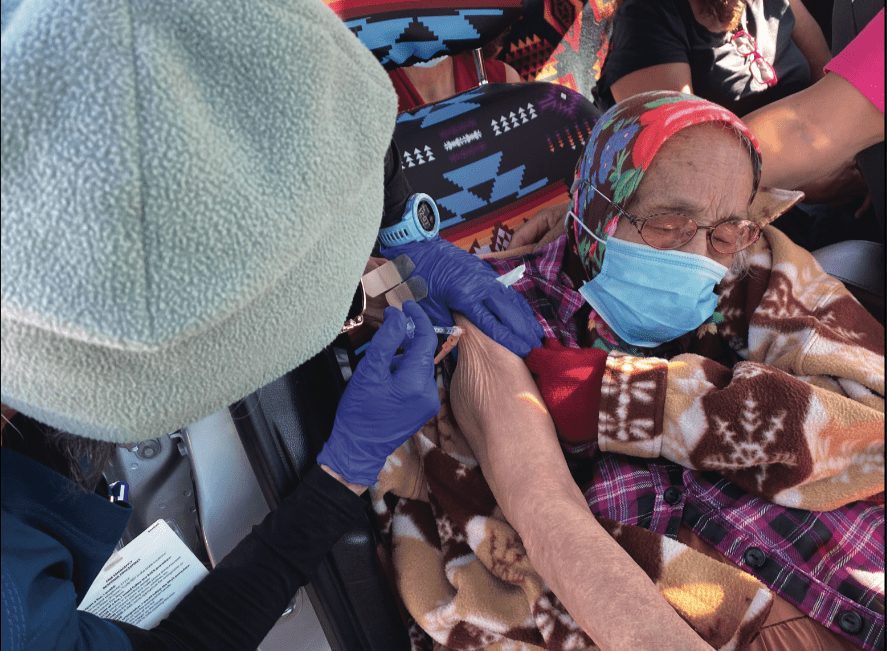
“When they have vaccines available, there are huge lines and people will wait all day in their cars. You’ll see the lines going for miles,” she said. She described that her own family’s losses amplified the importance of the vaccine.
“My brother got vaccinated…. For him there was an urgency in getting it because of losing family members,” she said. “I have other family members that want to get vaccinated, but they don’t live on a reservation, so they have to wait.”
In Mahnomen County, completely situated within the boundaries of the White Earth Indian Reservation in northwest Minnesota, 85 percent of residents aged 65 and older have been vaccinated, one of the highest rates in the state, public radio reported last week.
Minnesota’s state reporting on Native Covid-19 is among the best of the 50 states, according to the Urban Indian Health Institute.
Experts attribute the positive outcomes to close collaboration between reservation and county officials, as well as large vaccination allocations.
However, data collection and analysis of AI/NA pandemic still “has resulted in a substantial gap in understanding the disproportionate impact of COVID-19 on people of color across the U.S.,” the institute complained.
“This is a data genocide on Native people,” said Abigail Echo-Hawk, director of the institute. “American Indians and Alaska Natives are dying at disproportionate rates and decision makers don’t even have accurate data to ensure we are properly funded and resourced,” she said.
Contact Justine Anderson at [email protected]
- As temps rise, so do water protector arrests - March 31, 2021
- Navajo Nation: From No. 1 in infections to No. 1 in vaccinations - February 26, 2021
- ‘Honor the Earth’ vs. Enbridge Line 3 Oil Pipeline - January 13, 2021